The liver is an organ that performs many different functions in the human body. In particular, it is a biological “filter” that collects blood from the intestines through the portal vein and cleanses it of toxic substances.
With cirrhosis and liver cancer, the pressure in the portal vein increases - a condition develops that doctors call portal hypertension. It causes fluid to accumulate in the abdominal cavity and ascites develops. [1.15]
- Causes of ascites in cirrhosis and liver cancer
- Ascites in pancreatic cancer
- Symptoms of ascites in cirrhosis and liver cancer
- Treatment of ascites in cirrhosis and liver cancer
- Prices
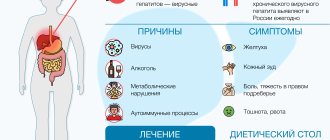
About the organ and the disease
The liver is a multifunctional organ. One aspect of her work is cleansing the body. Being a kind of filter, the liver collects blood from the intestines through the portal vein and cleanses it of toxins.
The most serious organ disease is cirrhosis. It is a pathological process in which healthy tissues die and are replaced by fibrous ones. Such damage is so serious that it is irreversible and leads to a complete cessation of organ function.
As for ascites, this pathology is characterized by excessive accumulation of liquid masses in the abdominal cavity. It is secondary in nature, and complicates cirrhosis of the liver and some other diseases.
If the necessary medical care is not provided in time, the disease will be accompanied by electrolyte disturbances and protein loss. This entails a deterioration in the functioning of internal organs, which greatly aggravates the prognosis of the underlying disease.
Ascites in liver cirrhosis begins to develop due to a significant increase in pressure in the portal vein.
In the normal state of the peritoneum, a small amount of fluid is constantly present in it; the peritoneum absorbs it back without problems.
An excessive increase in pressure in the portal vein gives impetus to a whole cascade of pathological reactions. They lead to an imbalance in the functioning of the peritoneum: it is simply no longer able to absorb liquid. Thus, liquid masses accumulate in the abdominal cavity.
Pathogenetic approaches to diuretic therapy of ascites in patients with liver cirrhosis
Ascites is one of the most significant complications of liver cirrhosis, occurring in approximately 40–50% of patients within a 10-year period from diagnosis. The development of ascites is considered an important unfavorable prognostic sign of disease progression, as it is associated with 50% mortality over the next two years [23, 26].
To date, the mechanisms of ascites formation in liver cirrhosis remain unclear. How does fluid accumulate in the abdominal cavity, what is the physiological essence of this process, what is its connection with central hemodynamics, the condition of the kidneys and peritoneum? Why is this particular syndrome a turning point in the lives of patients with cirrhosis and, regardless of the etiology of the disease, determines the further survival and quality of life of these patients?
In addition, the progressive growth of the pharmacological market is almost not noticeable in hepatology. Whereas in other areas of medicine, for example, in cardiology, consensus documents on the treatment of patients with heart failure (HF) are annually adopted, which include new diuretic drugs, and optimize regimens and approaches to therapy. Treatment of edematous-ascitic syndrome in a cardiac patient has been clearly established, while discussion of the principles of supervision of a hepatological patient entails a number of disputes and disagreements.
These and many other questions already require resolution today, primarily for medical specialists who are involved every day in the treatment of patients with chronic liver diseases.
Mechanisms of ascites in patients with liver cirrhosis
The development of ascites is caused by increased lymph production in the liver due to the blockade of the outflow of venous blood from it, but its occurrence begins from the moment of damage to hepatocytes, i.e., from the stage of hepatitis.
The main mechanisms for the development of edematous-ascitic syndrome are (
):
- liver dysfunction (hepatoprivate syndrome);
- release of vasodilators and cytokines by damaged hepatocytes;
- activation of the sympathoadrenal (SAS) and renin-angiotensin-aldesterone system (RAAS) with subsequent dysfunction of the cardiovascular system (CVS) and kidneys;
- formation of portal hypertension (PH): • due to activation of cells of the sinusoidal compartment with the development of functional PH; • activation of fibrogenesis processes in the liver with disruption of its vascular bed and the development of organic PG;
- blockade of venous and lymphatic drainage from the liver.
Let us take a closer look at these provisions.
Development of hepatic cell failure syndrome (HCF) in patients with liver cirrhosis. Characterized by:
- disruption of protein synthesis and the development of hypoalbuminemia, which leads to a decrease in the oncotic pressure of the blood plasma, while the release of fluid from the vascular bed increases, the volume of intravascular fluid decreases, the filling of the central arterial bed decreases (effective circulating blood volume (BCV)), which compensatory increases the activity of the RAAS and increases the level of aldosterone, which causes fluid retention. However, in conditions of persistent liver pathology, the compensatory mechanism (activation of the RAAS) becomes pathological, contributing to further fluid retention in the body, the formation of ascites and edema;
- disruption of the detoxifying function of the liver, which is accompanied by a disorder of hormone catabolism, an increase in the content of estrogens in the blood, which have an antidiuretic effect and stimulate fluid retention and activation of the RAAS.
Release of vasodilators and cytokines by damaged hepatocytes. Impairment of the detoxifying function of the liver, the development of PCN and porta-caval shunting contribute to the penetration into the blood from damaged hepatocytes of vasodilators, such as glucagon, nitric oxide, prostaglandin E2α, atrial natriuretic hormone, vasointestinal peptide, prostacyclin, which leads to generalized vasodilation and a decrease in overall peripheral vascular resistance (PVR). At the same time, powerful vasoconstrictors, in particular endothelin-1, are synthesized in the endothelium of liver vessels, under the influence of endotoxins and cytokines, which causes vasospasm. That is, there is a disconnection of local and general blood flow associated with an imbalance of vasodilating and vasoconstrictive substances, which leads to:
- to the activation and transformation of Ito sinusoidal cells into myofibroblasts, which contract, narrow the lumen of the sinusoids, forming a functional PG, together with Kupffer cells they synthesize collagen and vasoactive substances that stimulate the SAS and RAAS;
- to inadequate peripheral vasodilation, causing compensatory activation of the SAS and RAAS, and an increase in the level of antidiuretic hormone (ADH).
Activation of SAS and RAAS. Activated SAS and RAAS affect the main targets:
- CVS: the consequence of peripheral vasodilation is an increase in blood volume, stroke volume (SV), minute volume of blood flow (MCV) and the formation of a hyperkinetic type of blood circulation. The hyperkinetic state of central hemodynamics initially has a compensatory nature, aimed at increasing the central effective volume of circulating blood and intrahepatic blood flow, which prevents a decrease in portal pressure with the development of portosystemic collaterals. However, already in the early stages, this type of hemodynamics leads to functional overload of the myocardium, contributing to the development of diastolic and subsequently systolic dysfunction, realizing systemic manifestations of the disease in the form of heart failure and ascites [20, 22, 24, 37];
The main factors affecting the CVS in liver cirrhosis are blood shunting with a direct toxic effect on the myocardium of biologically active substances (adrenaline, histamine, serotonin), dysmetabolic disorders associated with impaired liver function, autonomic disorders, prolonged hyperactivation of the SAS and RAAS [7, 35, 38 ]. A combination of metabolic disorders of biologically active substances leads to the development of so-called metabolic cardiomyopathy with dilatation of the heart cavities and heart failure. This condition is aggravated by chronic functional overload of the heart against the background of a hyperkinetic type of blood circulation [2, 4, 6]. That is, with the development of liver disease, a systemic reaction develops, which is realized through the involvement of the cardiovascular system in the process, forming methods of compensation and decompensation similar to heart failure with the occurrence of edematous-ascitic syndrome [11, 12, 34].
- Kidneys: decreased blood flow in the cortex against the background of a hyperdynamic type of blood circulation, which leads to vasoconstriction, release of renin and increased aldosterone levels. Compensatory for the restoration of bcc, these systems stimulate an increase in the reabsorption of sodium and water, causing the transition of fluid into the intercellular space, which leads to the formation of ascites and edema [5, 8].
The main factors of kidney damage in liver cirrhosis are:
- • reduction in renal blood flow and perfusion of the renal cortex as a result of blood shunting through anastomoses in the subcortical layer;
- • decrease in effective BCC;
- • increased levels of vasoconstrictors (endothelin-1, thromboxane, etc.);
- • decreased synthesis of prostaglandins and kallikrein by the kidneys, which have a vasodilating effect.
Renal damage occurs as a result of an imbalance between systemic vasodilation and renal vasoconstriction. Despite the systemic vasodilation characteristic of liver cirrhosis, vasoconstriction occurs in the kidneys, as in the liver, which leads to a decrease in the glomerular filtration rate, while the level of renin in the plasma increases. Sodium is compensatoryly reabsorbed in the renal tubules, which causes an increase in urine osmolarity. Fluid accumulates in the body, despite normal urine volume, a low-salt diet and diuretic therapy. In extrarenal vessels, dilatation of the arteries predominates, and as a result, OPS decreases with the development of arterial hypotension. Cardiac output is unchanged or even increased, but effective renal blood flow is reduced as a result of redistribution of blood flow to the spleen, skin and other organs, thus shunting the renal cortex. The earliest sign of activation of the renal mechanism during the development of ascites in patients with liver cirrhosis is sodium retention in the body, which is manifested by a decrease in daily sodium excretion in urine to less than 78 mmol/day [8, 16].
Renal sodium retention is one of the likely causes of ascites, preceding the accumulation of ascitic fluid. In the early stages, it is the result of blockade of venous outflow from the liver and primary vasodilation.
Formation of GHGs. The development of a powerful imbalance of vasoactive substances, causing spasm of the sinusoids, as well as promoting active fibrogenesis in the liver, with the formation of cirrhotic nodes, leads to disruption of the venous bed of the liver and the development of PH.
The reversibility of ascites is determined by the stage of PG. Ascites is potentially reversible if there is a functional PH, and irreversible if changes in the vascular bed of the liver have occurred and organic PH has formed [1, 11].
Functional (sinusoidal) PG is determined [19, 23, 38]:
- vegetative tone;
- contraction of Ito cells and, as a consequence, narrowing of the lumen of the sinusoids and their release of vasoactive substances that stimulate the SAS and RAAS;
- hepatic vascular tone, regulated by vasoactive substances;
- rheological properties of blood in the vessels of the portal system.
Organic PG is formed against the background of a violation of the cytoarchitecture of the liver, it is determined [23]:
- compression and destruction of sinusoids;
- portohepatic shunts;
- proliferation of connective tissue in the centrilobular zones of the lobules.
It is important to note that even at the stage of organic PG, its functional component is preserved, which can be reduced using drug therapy aimed at correcting the condition of the SAS, RAAS, blood rheology and other pathogenetic links.
Blockade of venous and lymphatic drainage from the liver. Increased pressure in the portal system leads to disruption of venous outflow from the liver and unpaired abdominal organs, which is accompanied by overflow of the sinusoids and increased lymph production in the liver.
In patients with liver cirrhosis, the volume of daily lymphatic drainage through the thoracic lymphatic duct can increase to 20 liters. Lymph from the vessels of the liver and unpaired organs sweats into the abdominal cavity, forms ascites, establishing a dynamic equilibrium with the process of its absorption into the intestinal capillaries.
Thus, we can conditionally distinguish several levels of ascites formation, closely interrelated:
- humoral-metabolic, determined by an imbalance of vasoactive substances (vasodilators and vasoconstrictors), hypoalbuminemia, diselectrolyte disorders, hyperestogenemia, an increase in ADH;
- cellular, determined by the specific response of liver cells (hepatocytes, endothelial cells, Kupffer, Ito cells) and peritoneum (mesotheliocytes);
- organ, determined by the initial state, involvement in the process and specific response of target organs (the liver itself, cardiovascular system, kidneys);
- systemic, determined by the nature of the neuroendocrine response of the SAS, RAAS and systemic implementation of PG.
Moreover, the reversibility of these changes depends on the stage of PG (functional or organic).
Classification of ascites
Depending on the amount of ascitic fluid and the effectiveness of therapy, the following are distinguished:
- initial or transient (up to 400 ml, detected by ultrasound);
- moderate (when ascites is not intense and responds well to therapy);
- severe or intense ascites;
- resistant ascites (a variant of tense ascites resistant to treatment).
The criteria for resistant (refractory) ascites are the absence of a decrease or a decrease in body weight of less than 200 g / day in the patient for 7 days against the background of a low-salt diet (5.2 g of table salt per day) and intensive diuretic therapy (spironolactone 400 mg / day and furosemide 160 mg/day), as well as a decrease in urinary sodium excretion to less than 78 mmol per day [16, 25]. Resistant ascites is also spoken of in cases where it does not decrease or quickly recurs after paracentesis or complications of diuretic therapy do not allow diuretics to be prescribed in effective doses. In practice, criteria for resistant ascites are detected in less than 10% of patients with liver cirrhosis.
The causes of resistant ascites are usually:
- excess sodium and fluid intake;
- inadequate diuretic therapy;
- hypotension;
- alkalosis;
- hypokalemia, hyponatremia, hypoalbuminemia;
- taking non-steroidal anti-inflammatory drugs;
- progression of liver disease;
- Budd–Chiari syndrome;
- peritoneal carcinomatosis;
- spontaneous bacterial peritonitis (SBP).
Many causes of refractory ascites are potentially reversible, so their timely elimination can significantly increase the effectiveness of therapy.
Treatment of ascites in patients with liver cirrhosis
It should be noted that the task of treating ascites in patients with liver cirrhosis is more difficult than treating other forms of fluid accumulation in the body, because the formation of edematous-ascitic syndrome is a manifestation of significant decompensation of the disease. According to the results of controlled studies, the appearance of ascites significantly worsens the quality of life and increases the risk of developing fatal complications of liver cirrhosis [27, 39], so its therapy is one of the most important components of the successful treatment of these patients. However, given that complex neurohormonal mechanisms are involved in the development of ascites, thoughtless dehydration can only cause side effects and “rebound” fluid retention.
Regimen, diet and fluid intake in patients with liver cirrhosis and ascites. In patients with ascites who do not limit dietary salt intake, daily urinary sodium excretion is reduced to 78 mmol or less, while extrarenal sodium losses can reach 10 mmol/day.
Consumption of more than 90 mmol/day of sodium by patients with liver cirrhosis leads to the development of ascites, since each gram of sodium retains up to 200 ml of fluid. Therefore, it is recommended to consume no more than 90 mmol of sodium (5.2 g of table salt) with food during the day, in combination with limiting the amount of liquid to 1 liter per day. It is important to take into account that fluid restriction is not indicated for patients with low serum Na levels (less than 120 mmol/l) [16].
To date, there are no published studies that demonstrate a positive or negative effect of water restriction on the resolution of ascites. Most experts believe that there is no role for water restriction in patients with uncomplicated ascites. Despite this, a water-restricted diet for patients with ascites and hyponatremia has become standard clinical practice in many centers. There is a lot of controversy on this issue, and the best approach has not yet been found. As a rule, hepatologists treat such patients with strict water restriction. From the point of view of the pathogenesis of hyponatremia, such treatment is counterintuitive and may worsen the severity of central hypovolemia, which triggers non-osmotic ADH secretion. An even greater increase in the concentration of circulating ADH leads to a further decrease in renal function. Impaired free water clearance is present in 25–60% of patients with cirrhotic ascites, and they often develop spontaneous hyponatremia.
Errors in diet often cause difficult to treat (resistant, refractory) ascites. If you consume a large amount of salt, the use of modern diuretics, even in high doses, will be ineffective.
The diet should be essentially vegetarian as most high protein foods (meat, eggs and dairy) are high in sodium, so the diet should therefore be supplemented with low sodium protein foods. It is recommended to eat salt-free bread, butter and cook all dishes without adding salt. Products rich in potassium and microelements are also shown. The energy value of the diet should be ~1500–2000 kcal, containing 70 g of protein and 90 mmol of sodium per day.
A patient with ascites is recommended to limit physical activity, which helps reduce the amount of metabolites produced in the liver. Also, in the supine position, portal venous and renal blood flow slightly increases.
General approaches to the treatment of ascites in patients with liver cirrhosis. Strategic directions for the treatment of ascites include limiting salt in food and drug removal of excess fluid from the body. In addition, based on the considered positions of the pathogenesis of ascites in patients with liver cirrhosis, it is important to solve therapeutic problems of correcting PG, PKN, blocking peripheral vasodilators, suppressing the activity of the SAS and RAAS, normalizing the function of the cardiovascular system, kidneys, etc.
For safe drug removal of fluid from the body, three steps must be followed:
- Excess fluid must be transferred from the extracellular space into the vascular bed.
- Excess fluid must be delivered to the kidneys, where it can be filtered.
- When primary urine enters the renal tubules, reabsorption must be blocked, this will ensure the removal of excess fluid from the body [13].
To transfer excess fluid from the extracellular space into the vascular bed, the following are used:
- active diuretics (diuretics), which, by reducing blood volume and hydrostatic pressure, facilitate the transition of fluid from the extracellular space into the vascular bed;
- hemodynamically active neurohormonal modulators: beta blockers, angiotensin-converting enzyme inhibitors (ACEIs), angiotensin receptor antagonists (ARA) [4, 16];
- drugs that increase oncotic pressure in the blood (blood plasma and albumin preparations) and osmotic pressure (aldosterone antagonists, increasing ion exchange and reducing the severity of dilution hyponatremia).
The most optimal beta-blockers in patients with liver diseases, the effectiveness of which is confirmed by the results of a meta-analysis, are non-selective derivatives of the propranolol group - Anaprilin in an individually selected dose - 40-80 mg / day or carvedilol in an individual dose - 25-50 mg / day [3, 14, 28, 31].
Among ACEIs in patients with liver cirrhosis, the drugs of choice are the lisinopril group in an individually selected (2.5–20 mg/day) dose or the dual-excretion drug spirapril 6 mg/day.
Unlike other representatives of this class, they are a ready-made dosage form, and their effectiveness is confirmed by the results of comparative studies [11, 17].
Among the ARAs, eprosartan can be used in this category of patients in an individually selected dose - 300–600 mg/day. Open studies have demonstrated the effectiveness of drugs of this group in patients with liver cirrhosis [32, 40].
Positive inotropic agents are used to deliver excess fluid to the kidneys:
- cardiac glycosides, the criterion for prescribing them in patients with liver cirrhosis is the presence of normal or reduced ejection fraction (EF) (due to the initial hyperkinetic state of central hemodynamics in these patients with increased cardiac output) during ECHO-CG, as well as atrial fibrillation;
- Neoton (for the purpose of metabolic support of the myocardium).
To improve renal filtration, the following are recommended:
- dopamine (better for arterial hypotension; due to its effect on dopaminergic receptors, this drug increases the proportion of renal blood flow);
- Eufillin (with systolic blood pressure (SBP) above 100 mm Hg).
To block the reabsorption of primary urine in the renal tubules, diuretics themselves are used (mainly loop diuretics and aldosterone antagonists).
Diuretic therapy for patients with liver cirrhosis and ascites. Taking into account the complex pathogenesis of the development of edematous-ascitic syndrome, diuretics of various pharmacological groups are used in its treatment: aldosterone receptor antagonists, potassium-sparing, loop, thiazide diuretics and carbonic anhydrase inhibitors. The algorithm for prescribing diuretics to patients with liver cirrhosis is presented in Scheme 1.
The effect of diuretics in liver cirrhosis and ascites is multifaceted and consists of their influence on renal structures and extrarenal mechanisms for regulating water and electrolyte balance [9, 10], including effects at the level of:
- cell membranes - diuretics regulate their permeability, the functions of intracellular transport proteins and the electrochemical processes of ion transport;
- individual nephron - influence on the filtration load of the nephron, the transport function of its various segments;
- kidneys - influence on intrarenal hemodynamics, internephron relationships, activity of tissue components of neurohumoral systems;
- systemic hemodynamics and water-electrolyte balance.
The main principle of unloading therapy for edematous-ascitic syndrome in patients with liver cirrhosis is to obtain a gradually developing and stable diuretic effect, with spironolactone being the drug of choice [15, 23].
In cases of refractoriness to therapy with aldosterone antagonists, before prescribing other diuretics acting on other parts of the nephron, it is advisable to evaluate the indications for the use of additional therapeutic measures, in particular for the administration of albumin and blood-substituting colloid solutions.
With severe edematous-ascitic syndrome, the scope of diuretic therapy can be expanded with loop or thiazide diretics, which suppress the reabsorption of sodium and water.
The combined administration of potassium-sparing and potassium-sparing diuretics is recommended, which helps reduce the risk of electrolyte disturbances [18, 21, 29].
The dosage and frequency of taking the drug are selected individually for each patient. When a patient is admitted to hospital, it is recommended to determine daily sodium excretion, which facilitates the selection of a diuretic and monitoring the effect of treatment [16].
At initial signs of ascites, therapy begins with one of the drugs from the group of potassium-sparing diuretics, usually spironolactone. If ineffective, a loop diuretic is added.
The presence of signs of severe ascites requires the initial use of combination therapy, with spironolactone prescribed as a reliable partner for loop diuretics.
In patients with liver cirrhosis with moderate and severe PH, it is possible to begin treatment with courses of aldosterone antagonists even before the formation of ascites in minimal (25–50 mg/day) dosages that do not change diuresis as a neurohumoral modulator, but this point of view is the author’s and has not been confirmed by wide clinical trials.
In case of decompensation of liver cirrhosis (in the form of development of ascites), the use of spironolactone is absolutely necessary and there is no need to be afraid of its combination with ACE inhibitors or ARAs if, in parallel, active diuretics are correctly used to achieve positive diuresis. The drug is taken in high doses (100–300 mg, given once in the morning or in two doses in the morning and afternoon) for a period of 1–3 weeks until compensation is achieved. After this, the dose of spironolactone should be reduced.
It must be remembered that the concentration of spironolactone in the blood plasma reaches a plateau by the third day of treatment and after discontinuation (or reduction of the dose of the drug), its concentration and effect disappears (decreases) after three days. After compensation is achieved, the use of high doses of spironalactone is stopped and the issue of prescribing small doses of the drug as an additional neurohormonal modulator is considered.
For long-term maintenance therapy of patients with liver cirrhosis, it is recommended to use small (25–50 mg) doses of spironolactone in addition to ACE inhibitors and beta-blockers (BAB), which allows for more complete blocking of the RAAS and SAS.
In cases where it is necessary to replace spironolactone, the drug of choice is amiloride 10–15 mg/day.
The optimal ratio of spironolactone and furosemide is 5:2, for example, 100 mg of spironolactone and 40 mg of furosemide, etc. The maximum daily doses of these drugs are 400 and 160 mg, respectively.
Furosemide, in turn, may be ineffective in severe hyperaldosteronism, when sodium not reabsorbed in the loop of Henle is absorbed in the distal nephron. The second reason is hypokalemia and alkalosis.
Alternative, in cases of ineffectiveness, loop diuretics to furosemide for the treatment of ascites in patients with liver cirrhosis can be considered: Uregit (ethacrynic acid) 25–50 mg/day and bumetanide, which is not weaker than furosemide and is used in doses from 0.5 to 10 mg, which allows you to achieve optimal diuresis.
Ethacrynic acid and thiazides, as long-acting diuretics, are less indicated for patients with liver cirrhosis, since they can aggravate developed electrolyte disturbances, and even after their withdrawal, potassium loss in the urine and an increase in alkalosis may continue.
Therefore, in particular, thiazides are used primarily at the stage of maintenance therapy and/or the inability to use spironolactone. Taking into account possible side effects, thiazide diuretics in patients with liver cirrhosis are prescribed for a course of no more than 7-14 days with a break of 3-4 days.
In addition to the above, in 2006, one of the most effective and safe loop diuretics, torasemide (Diuver), was registered in Russia. Its starting dose is 5–10 mg, and if necessary, it can be increased to 20 mg per day. Torsemide not only has a more pronounced diuretic effect than furosemide, but also has its own activity in relation to aldosterone receptors, which provides it with a potassium-sparing effect. The advantage is the absence of undesirable effects of aldosterone antagonists (hyperkalemia, hirsutism and others), the drug has high bioavailability (80% versus 50% for furosemide), a prolonged effect (half-life 3-5 hours versus 1 hour for furosemide) and a mild hypotensive effect. The pharmacokinetics of torasemide is little dependent on renal function and intestinal condition, which provides a low risk of drug accumulation and lower excretion of potassium, calcium, inorganic phosphates and magnesium compared to furosemide.
In the treatment of edematous-ascitic syndrome in patients with liver cirrhosis, it is possible to use torasemide both as monotherapy and in combination with Veroshpiron. Torsemide therapy is indicated for decompensation of ascites, as well as for the prevention of its occurrence in dosages of 5–20 mg, which do not cause hypokalemia even with long-term use. It is recommended to use a stepwise approach, starting with 5 mg/day, increasing the dose by 5 mg every 2-3 days until the effect is achieved. At the outpatient stage, it is not recommended to exceed the daily dose of 20 mg, since a larger amount of the drug requires frequent monitoring of potassium levels.
To evaluate the effectiveness of diuretic therapy in patients with liver cirrhosis and ascites, a number of comparative studies of torasemide and furosemide were conducted. Thus, in a double-blind crossover study, the results of a single oral dose of furosemide (80 mg) and torasemide (20 mg) were compared in 14 patients. Torsemide was superior to furosemide in diuretic and natriuretic activity. Five patients had a weak response to furosemide, while torasemide caused a significant increase in natriuresis and diuresis [30, 33, 36].
Similarly, in a double-blind, randomized study of 28 patients with ascites treated with spironolactone (200 mg/day), the results of 6 weeks of therapy with torsemide (20 mg/day) and furosemide (50 mg/day) were compared. Both drugs had comparable effects on body weight, diuresis, and excretion of uric acid, sodium, and chloride, but excretion of potassium, calcium, inorganic phosphate, and magnesium was lower in the torsemide group [30, 33, 36].
A group of 46 patients with liver cirrhosis complicated by ascites (randomized trial) were treated with torasemide 20 mg/day or furosemide 40 mg/day in combination with spironolactone 200 mg/day. If it was not possible to achieve a weight loss of 300 g/day, the doses of diuretics were increased every 3 days to 40, 120 and 400 mg/day, respectively. Torsemide caused a more pronounced increase in diuresis than furosemide, although in general the treatment results in the 2 groups were comparable. An increase in diuretic doses was required in 2 patients in the torasemide group and in 9 patients in the furosemide group [33, 36].
That is, according to the results of studies, torasemide can be considered as an alternative to the combination therapy of Furosemide + Veroshpiron in patients with liver cirrhosis and ascites.
Carbonic anhydrase inhibitors have not found widespread use in patients with ascites, since their suppression of sodium and water reabsorption in the proximal tubule is compensated by its increase in the distal segments of the tubules.
Drugs in this group can be used as an adjuvant while taking active diuretics (loop and/or thiazide). Carbonic anhydrase inhibitors block the enzyme in the area of the proximal renal tubules, which is accompanied by slight diuresis (an increase of up to 10–15%), but this increases the “loading” of sodium in the underlying sections of the tubules, which increases the effectiveness of stronger diuretics. When the carbonic anhydrase enzyme is depleted after 3-4 days of continuous use, the activity of acetazolamide decreases, which requires a break in treatment.
Therefore, acetazolamide (Diacarb) is recommended at a dose of 0.25 g three times a day for 3-4 days with a two-week break. This therapeutic tactic helps to acidify the environment, restores the diuretic activity of thiazide and loop diuretics, with long-term use of which alkalosis develops. When combined with Eufillin, the diuretic effect of Diacarb increases.
To avoid the development of refractoriness and side effects of diuretics in patients with ascites, it is important to evaluate the effectiveness of treatment and conduct clinical and laboratory screening to determine indications for subsequent adjustment of the dosage regimen or discontinuation of drugs.
Read the continuation of the article in the next issue.
S. N. Mehdiev , Doctor of Medical Sciences, Professor Yu. A. Kravchuk , Candidate of Medical Sciences I. V. Subbotina O. A. Mehtieva * M. V. Shapovalov VMA named after. S. M. Kirova, *St. Petersburg State Medical Academy named after. I. I. Mechnikova , St. Petersburg
Symptoms
Symptoms of the disease can appear very quickly. We are talking, as a rule, about several days.
When examined by a doctor or by ultrasound, it is possible to determine the beginning of the process by a number of signs:
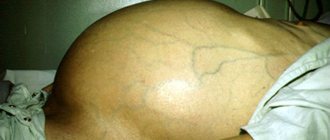
- Abdominal circumference increases;
- The skin becomes stretched;
- The navel (especially in thin people) protrudes forward;
- Striae form;
- The venous network is easily visible;
- If a person stands, the stomach hangs down;
- If it is in a lying position, it spreads to the sides and hangs down on the sides.
If the accumulation of liquid mass is significant, additional symptoms arise:
- Cough with phlegm;
- Shortness of breath, which worsens when lying down;
- Heaviness in the upper central area of the abdomen when eating food;
- Belching, nausea, vomiting;
- Stool disorders;
- Urination becomes more frequent;
- Swelling of the legs occurs.
The development of the listed symptoms is observed against the background of signs that indicate cirrhosis of the liver:
- Nausea;
- Bitterness in the mouth;
- Dull pain in the area of the right hypochondrium;
- Itching;
- Jaundice;
- Nosebleeds, etc.
Constipation
average life expectancy
How long do people with abdominal hydrops live? It is possible to determine the average life expectancy of a patient only based on the results of a biochemical blood test and instrumental examination of the liver. According to experts, a lot depends on the patient himself, who must strictly adhere to the drinking regime and diet.
Depending on the form of hepatic cirrhosis and the presence of associated complications, the following life expectancy is determined:
- compensated cirrhosis with initial ascites (no more than 1.5 liters of fluid) - more than 10 years;
- subcompensated cirrhosis with moderate ascites (no more than 4.5 l) - no more than 5-6 years;
- decompensated cirrhosis with massive ascites (more than 5 l) - no more than 1 year.
It is important to understand that it is impossible to determine the average life expectancy by the amount of fluid accumulated in the peritoneum. The prognosis depends on a number of factors - the stage of development of cirrhosis, the patient’s age, the effectiveness of treatment, compliance with the specialist’s instructions, etc.
Causes
An excessive increase in pressure in the portal vein is nothing more than portal hypertension. As it develops, the following pathological changes appear:
- The load on the venous and lymphatic vessels increases, which leads to sweating of the liquid mass through the vascular walls into the peritoneal cavity;
- The level of protein in the blood decreases, creating oncotic pressure, which helps retain the liquid mass in the vessels;
- The volume of circulating blood decreases, blood flow worsens, this affects all neighboring organs.
Experiencing these disruptions, the body as a system is forced to work to ensure that the blood vessels narrow and sodium and water are retained. But it turns out that as a result of this, even more liquid accumulates.
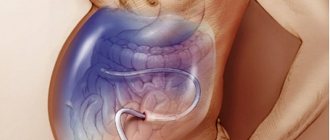
Technique for performing laparocentesis
A mini-intervention such as laparocentesis is performed under local anesthesia, with the patient often in a sitting position, sometimes placed on his back. The area where the puncture will be made is cleaned and sterilized. After administering the anesthetic, a special needle is used to make a puncture in the lower abdomen (approximately halfway between the navel and pubis), where a small tube is inserted. It will help remove liquid. The amount of fluid removed per procedure on average ranges from 3 to 5 liters, but in more severe cases the doctor may decide to remove 10 liters.
Laparocentesis usually takes about half an hour, but can take longer. The time will depend on the volume of fluid removed and the patient's condition.
After completion of the procedure, the puncture site is tightly bandaged. The patient's temperature, pulse, and blood pressure are always measured. Weight is measured before and after laparocentesis.
After laparocentesis, samples of the resulting fluid are examined to determine its origin (cytological examination). The patient will not have to look for an institution where they can examine the resulting liquid, because the Yusupov Hospital has its own laboratory.
If the fluid is edematous in nature, then this may indicate heart failure, liver cirrhosis or nephrotic syndrome. When receiving fluid of an inflammatory nature, one should talk about the presence of tumors or metastases in the abdominal organs.
Stages
There are 4 stages of cirrhosis, the 3rd and 4th of which are usually burdened by ascites:
- Compensation stage. The tissue of the organ has undergone changes, fibrosis is localized mainly in the periphery, portal hypertension and ascites are absent.
- Subcompensation stage. Fibrosis spreads from the periphery to the center of the liver, and portal hypertension develops. Ascites is still insignificant, symptoms of the disease begin to appear.
- Stage of decompensation. The amount of fibrosis increases and reaches between half and two-thirds of the liver volume. Ascites is rapidly progressing.
- Terminal stage. New symptoms are added, the prognosis for survival is very low, the patient’s condition is serious, and the ascites is excessive.
What liver diseases lead to dropsy of the abdomen?
Both cirrhosis and ascites result from long-term liver disease. While the reasons may be different. Liver damage can be caused by various agents:
- viruses,
- toxins,
- mechanical obstacles,
- volumetric processes in the organ itself and in the immediate vicinity of it,
- medicinal substances,
- congenital conditions
- autoimmune processes,
- metabolic disease.
There are diseases of other organs that also cause fluid effusion into the peritoneum: for example, tumor processes of the abdominal cavity and pelvis. Very rarely, the causes of cirrhosis cannot be determined, then it is called cryptogenic.
Treatment of ascites in cirrhosis
According to medical statistics, the vast majority (up to 90%) of patients with diagnosed ascites take diuretics and are on a special diet that helps restore water-salt balance.
Among the drugs used:
- Hepatoprotectors;
- Diuretics;
- Albumin and some others.
Surgery is performed if therapy is ineffective. This often happens with cancer patients. A separate group consists of patients with cancer in its later stages, in whom a large amount of fluid has accumulated in the abdomen.
In this case, to eliminate ascites, laparocentesis is used, which is puncture of the peritoneal wall with subsequent removal of fluid. Some of these patients require drainage. Through it, the accumulated liquid is evacuated within a few more days.
Intracavitary chemotherapy, in which the drug is injected directly into the peritoneal cavity, is also applicable to combat ascites against the background of cirrhosis.
Concluding the story about surgical interventions for cirrhosis aggravated by ascites, let’s name their varieties:
- If therapy is ineffective, laparocentesis is used;
- Shunting is performed to reduce pressure in the portal vein.
- Organ transplant.
Forecast
Ascites in cancer significantly worsens the general well-being of the patient. As a rule, such a complication occurs in the later stages of oncology, in which the survival prognosis depends on the nature of the tumor itself and its distribution throughout the body.
Life expectancy with ascites depends on the following factors:
- Functioning of the kidneys and liver;
- Activities of the cardiovascular system;
- The effectiveness of therapy for the underlying disease.
The development of ascites can be prevented by an experienced doctor observing the patient. Doctors at the Yusupov Hospital have extensive experience in dealing with various types of cancer. Qualified medical personnel and the latest equipment allow for accurate diagnosis and high-quality, effective treatment in accordance with European standards.
Survival prognosis
To predict the life expectancy of a patient with cirrhosis aggravated by ascites, it is necessary to take into account the advanced stage of the disease.
With continued exposure to unfavorable factors on the organ, cirrhosis worsens, which negatively affects survival.
World statistics show that patients with compensated liver cirrhosis can live more than ten years. If we are talking about decompensated cirrhosis, then up to 40% of patients die within the first three years, three years from the moment the disease is diagnosed.
The Onco.Rehab integrative oncology clinic offers modern methods of treating diseases according to international protocols.
Preparation for the laparocentesis procedure
Before laparocentesis, the doctor prescribes a number of necessary tests and diagnostic procedures, including:
- physical examination;
- blood clotting test;
- X-ray examination;
- Ultrasound;
All diagnostic procedures can be completed on site, because the equipment of the Yusupov Hospital is at its best. It has all the necessary latest equipment, which allows you to quickly and accurately establish a diagnosis with minimal negative impact on the patient’s body.
The patient should also tell the doctor if they are allergic to medications, pregnant, or if they are already taking medications. Immediately before the procedure, you need to empty your bladder and bowels, and do not eat or drink 12 hours before the operation.
Possible complications
After laparocentesis, hematomas may remain on the abdominal wall and discharge from the puncture site may be observed. Possible in theory
- intestinal damage;
- infection;
- bleeding due to damage to a large blood vessel;
- decreased blood pressure, dizziness, fainting (with simultaneous evacuation of too much fluid);
- dysfunction of the liver and kidneys.
However, if the procedure is performed by experienced specialists with proper training, complications during laparocentesis are extremely rare.
+7
Call or leave a request
Request a call!
What symptoms should you pay attention to?
- In the first stage of the disease, there are practically no complaints. There may be a bitter taste in the mouth or an unpleasant taste, or loss of appetite. The liver may be enlarged due to fatty degeneration, but it may be reduced or normal (the doctor can determine this during examination, according to ultrasound data).
- The second stage is characterized by increased symptoms. This is bloating, increased intestinal motility or rumbling, and sometimes loose stools. A “liver” tongue often becomes noticeable: lacquered, with no coating. And also “liver” palms of a red-burgundy color.
- When the disease decompensates, yellowing of the skin, discoloration of feces and darkening of urine, and the appearance of “bruises” occur. Vascular elements like asterisks or pinpoint hemorrhages appear throughout the body. In men, impotence occurs, gynecomastia (enlargement of the mammary glands) is possible, and in women, cycle disorders occur. If an infection occurs, an increase in body temperature is possible.
- The fourth stage of the disease, in which a clinical picture of a serious condition is formed. These are all of the above symptoms plus a blood clotting disorder, manifested by increased bleeding. Bleeding can be quite massive: for example, gastric or bleeding from varicose veins of the esophagus. The patient loses weight and develops digestive disorders. Severe weakness appears. Within a few days, a significant increase in the abdomen is possible. A pattern of varicose veins appears on the surface of the abdomen, called the “head of a jellyfish.”
If the patient is laid down, the shape of his abdomen will change. In a standing position, the stomach is round, hanging down, and when the patient lies on his back, his stomach “spreads” to the sides, becoming like a “frog” (flat).
Is a positive symptom of fluctuation. If you sharply press on the stomach from the side, you will feel the impact of a “wave” on the other side.
It is characteristic that the patient, who has visually lost a lot of weight, nevertheless maintains the same weight or even gains even more. This is due to the fact that several liters of accumulated fluid increases the patient’s weight.
At stage 4 of cirrhotic degeneration of the organ, problems with the lungs arise due to venous stagnation, which continues to progress. Shortness of breath and cough occur. They intensify in the lying position, when the fluid, spreading in the abdomen, begins to put pressure on the diaphragm.
When a large volume of effusion accumulates, the following problems may arise:
- With strong pressure on the abdominal wall, the formation of various hernias is possible: umbilical, inguinal, linea alba.
- Bleeding from dilated veins of the esophagus, bleeding from dilated veins of the stomach.
- Release of fluid into the pleural cavity (hydrothorax).