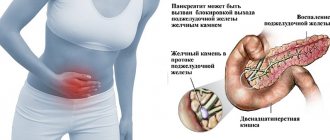
Chronic pancreatitis (CP) is a long-term inflammatory disease of the pancreas, with manifestations in the form of irreversible changes in the structure of the organ, which cause pain and/or a persistent decrease in its function.
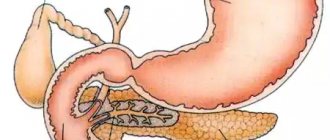
The pancreas performs important functions:
- secretion of most digestive enzymes
- production of insulin (a hormone whose deficiency develops diabetes mellitus)
There is a worldwide trend toward an increase in the incidence of acute and chronic pancreatitis, more than doubling over the past 30 years.
Reasons for the development of pancreatitis
The most common cause of chronic pancreatitis is alcohol consumption, and the quality and raw materials from which the drink is made do not matter.
Other reasons
- Toxins and metabolic factors:
- alcohol abuse
- smoking
- increased calcium levels in the blood (develops in patients with a tumor of the parathyroid glands)
- overeating and eating fatty foods
- protein deficiency in food
- effects of medications and toxins
- chronic renal failure
- Blockage of the pancreatic duct:
- stones in this channel
- due to dysfunction of the sphincter of Oddi
- blocking of the duct by a tumor, cysts
- post-traumatic scars of the pancreatic ducts (complication of endoscopic procedures: papillosphincterotomy, stone removal, etc.)
- Pathology of the gallbladder and biliary tract.
- Pathology of the duodenum.
- Consequences of acute pancreatitis.
- Autoimmune mechanisms.
- Heredity (gene mutations, 1-antitrypsin deficiency, etc.).
- Helminths.
- Insufficient oxygen supply to the pancreas due to atherosclerosis of the vessels supplying blood to this organ.
- Congenital anomalies of the pancreas.
- Idiopathic chronic pancreatitis (the cause cannot be determined).
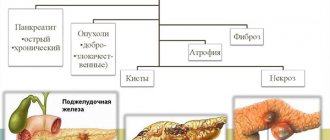
Classification and types
Many classifications of pancreatitis have been created according to various criteria.
In accordance with the international classification of diseases, there are:
- acute pancreatitis (ICD-10 code K85);
- chronic pancreatitis of alcoholic origin (ICD-10 code K86.0);
- other chronic pancreatitis (ICD-10 code K86.1).
Variants of acute pancreatitis:
- edematous with rapidly developing dysfunction of the gland;
- necrotic (pancreatic necrosis) - a more severe form, accompanied by the breakdown of organ tissue under the influence of its own enzymes.
Types of chronic inflammatory process of the pancreas:
| Variety | Cause | Peculiarities |
| Calcifying (calcifying) | Alcohol consumption | Chronic damage to the smallest pancreatic ducts causes the formation of plugs in them, which gradually calcify |
| Obstructive | Gallstone disease, tumor, scar deformity | Occurs when large ducts are compressed; cells are damaged secondary to increased intraductal pressure |
| Parenchymal-fibrous | Autoimmune process, recurrent inflammation | Rarely occurs, accompanied by widespread damage to glandular cells |
Chronic pancreatitis can be asymptomatic, but more often there is an alternation of remissions and exacerbations. During remission the patient has no complaints. Exacerbation of the chronic inflammatory process is accompanied by the appearance of symptoms of the disease.
Symptoms of pancreatitis
- abdominal pain: usually the pain is localized in the epigastrium and radiates to the back, increasing after eating and decreasing when sitting or bending forward
- nausea, vomiting
- diarrhea, steatorrhea (fatty stool), increased stool volume
- bloating, rumbling in the stomach
- weight loss
- weakness, irritability, especially on an empty stomach, sleep disturbance, decreased performance
- the symptom of “red drops” is the appearance of bright red spots on the skin of the chest, back and abdomen.
If such symptoms appear, it is recommended to undergo examination to exclude chronic pancreatitis.
Complications of chronic pancreatitis
If left untreated, possible complications of chronic pancreatitis include:
- diabetes
- vitamin deficiency (mainly A, E, D)
- increased bone fragility
- cholestasis (with and without jaundice)
- inflammatory complications (inflammation of the bile ducts, abscess, cyst, etc.)
- subhepatic portal hypertension (fluid accumulation in the abdominal cavity, enlarged spleen, dilation of the veins of the anterior abdominal wall, esophagus, liver dysfunction)
- effusion pleurisy (fluid accumulation in the membranes of the lungs)
- compression of the duodenum with the development of intestinal obstruction
- pancreas cancer.
Severity of chronic pancreatitis
There are three degrees of severity of chronic pancreatitis:
Mild degree
- exacerbations are rare (1-2 times a year), short-lived
- moderate pain
- no weight loss
- no diarrhea, no fatty stools
- Coprological examination of stool is normal (no neutral fat, fatty acids, soaps)
With mild severity of chronic pancreatitis, long courses of medication are usually not required, since lifestyle changes and giving up bad habits often prevent relapses.
Average degree
- exacerbations 3-4 times a year, occur with prolonged pain syndrome
- There may be an increase in amylase and lipase in the blood
- periodic loose stools, greasy stools
- there are changes in the coprogram
With moderate severity of chronic pancreatitis, a strict diet, longer courses of therapy, and constant supervision by the attending physician are necessary.
Serious condition
- frequent and prolonged exacerbations with severe, prolonged pain syndrome
- frequent loose stools, fatty stools
- loss of body weight, up to exhaustion
- complications (diabetes mellitus, pseudocysts, etc.)
In severe cases of chronic pancreatitis, constant maintenance therapy, stronger medications and a strict diet are required. Often, patients need careful monitoring not only by a gastroenterologist, but also by doctors of other specialties (endocrinologist, surgeon, nutritionist). Emerging exacerbations, as well as complications of the disease, pose a threat to the patient’s life and, as a rule, are an indication for hospitalization.
The presence of chronic pancreatitis, regardless of severity, requires immediate consultation with a doctor, since without treatment and lifestyle changes, the process will steadily progress.
Features of taking medications for pancreatitis
For pancreatitis, any self-medication is strictly contraindicated, even taking painkillers. The doctor determines the method of treatment, selects medications and their dosage strictly individually for each patient. The duration of treatment depends on the form of the disease, its severity, as well as on the patient’s body’s response to a particular drug. It is important not to forget about the medicine: take medications regularly and at the strictly designated time.
Photo: pressfoto / freepik.com
Diagnosis of pancreatitis
The EXPERT Clinic has an algorithm for diagnosing chronic pancreatitis, which includes:
Laboratory methods:
- A clinical and biochemical blood test is performed (of particular importance is the level of pancreatic enzymes in the blood - amylase, lipase)
- coprogram - the presence of certain substances in the stool (fats, soaps, fatty acids, etc.) is assessed. Normally, they should be absent, but in chronic pancreatitis, due to insufficient production of enzymes by the gland to break down these substances, they remain undigested and are detected in the feces
- fecal elastase is an enzyme of the pancreas, the level of which decreases when it is not working enough
- in certain cases, it is important to determine cancer markers
- If a hereditary genesis of the disease is suspected, a genetic examination of the patient is carried out.
Instrumental studies
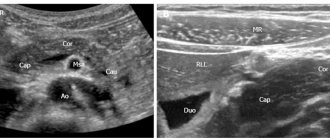
- Ultrasound of the abdominal cavity. Signs of inflammation of the pancreatic tissue, the presence of stones in the ducts, calcifications, cysts, and tumors of the pancreas are assessed. Additionally, changes in other organs of the gastrointestinal tract are determined to exclude complications of the disease, as well as concomitant pathologies.
- Elastography of the pancreas.
Allows you to determine whether there is fibrosis (hardening) of the pancreas, which is a criterion for the severity of structural changes in the organ. Ultrasound with elastography of a healthy pancreas - FGDS. Visualization of the duodenum is necessary to assess the presence of inflammation in it, as well as indirect signs of pancreatitis. It is necessary to exclude inflammation and pathological formations (tumor, diverticulum) in the area of the large duodenal nipple (through it, pancreatic secretions enter the duodenum; when it is blocked, the outflow of this secretion is disrupted, which leads to inflammation of the gland tissue). Visualization of the stomach and esophagus is necessary to exclude erosions, ulcers, and inflammation in them. Pathological changes in these organs are often combined with chronic pancreatitis, being mutually aggravating conditions.
- Additionally, CT and MRI of the abdominal cavity with cholangiography and RCHP may be prescribed. They are necessary to confirm the diagnosis, and are also prescribed if there is a suspicion of the presence of pathological formations in the pancreas, blockage of the gland ducts with a stone, tumor or cyst.
Treatment of pancreatitis
The main treatment for chronic pancreatitis is diet and giving up bad habits, lifestyle changes, as well as medications:
- drugs that reduce the production of hydrochloric acid by the stomach (proton pump inhibitors)
- enzyme preparations
- antispasmodics
- in the presence of pain - analgesics, NSAIDs; if the pain is extremely severe and is not eliminated by these drugs, narcotic analgesics are prescribed.
It is necessary to identify during the initial examination the pathology of other organs of the gastrointestinal tract (cholelithiasis, chronic cholecystitis, gastritis, duodenitis, peptic ulcer, hepatitis, bacterial overgrowth syndrome, intestinal dysbiosis, kidney disease, etc.), since these diseases may be the cause and/or aggravating factors of chronic pancreatic inflammation. In this case, treatment of other gastrointestinal diseases is necessary. The decision on the urgency and procedure for treating a particular concomitant disease is made by the attending physician.
If medications taken by a patient for other diseases may contribute to the development of the disease, the issue of replacing medications is decided.
All types of drug therapy should be prescribed and monitored by a gastroenterologist.
If any mechanical obstruction to the outflow of bile is detected, surgical treatment is indicated for the patient.
How long does the attack last?
Chronic pancreatitis in the acute phase can be accompanied by severe pain and a significant deterioration in health. However, not all patients experience such severe pain, but instead they suffer from other symptoms: lack of appetite, high fever, vomiting, diarrhea, etc.
But how long does the acute phase last? Doctors do not give a definite answer, since the duration of the attack is influenced by many factors, for example, the reasons that led to the development of this pathology or the presence of concomitant ailments. On average, during an exacerbation of pancreatitis, an attack lasts 1-2 hours or more than a day.
Forecast
Chronic pancreatitis is a serious disease. However, if you follow the recommendations of the supervising physician for the prevention of exacerbations (compliance with dietary recommendations, preventive courses of treatment, etc.), chronic pancreatitis proceeds “calmly”, without frequent exacerbations and has a favorable survival prognosis.
If the diet is violated, alcohol intake, smoking and inadequate treatment, degenerative processes in the gland tissue progress and severe complications develop, many of which require surgical intervention and can be fatal.
Progression of the acute period
Unfortunately, it is completely impossible to get rid of chronic pancreatitis, since this disease cannot be treated. How often it can flare up depends on the patient’s lifestyle. If he strictly follows all the doctors’ recommendations outside of an exacerbation and constantly adheres to a therapeutic diet, then acute periods occur extremely rarely.
Errors in nutrition are the main cause of exacerbation of pancreatitis
In situations where the patient does not follow a diet and neglects prevention, this becomes the reason for the progression of the disease and its frequent exacerbation. In this case, not only a deterioration in the general condition is observed, but also the appearance of symptoms characteristic of collapse and toxic shock. These include:
- weakness;
- paleness of the skin;
- dizziness;
- hot flashes of cold sweat;
- decreased blood pressure;
- oxygen starvation;
- temperature.
If all these symptoms appear, the patient must be urgently taken to a medical facility. If he is not provided with timely medical assistance, this can cause not only complications of the disease, but also death.
Prevention and recommendations
Prevention is based on eliminating risk factors that provoke the disease:
- timely treatment of diseases that provoke pancreatitis
- eliminating the possibility of chronic intoxication that contributes to the development of this disease (industrial, as well as alcoholism)
- ensuring a balanced diet and daily routine.
Nutrition for chronic pancreatitis
For pancreatitis, all dishes are made from lean meat and fish - and then only in the boiled version. Fried foods are prohibited. You can consume dairy products with a minimum percentage of fat content. It is advisable to drink only natural juices, compotes and tea from liquids.
The following should be completely excluded:
- all types of alcohol, sweet (grape juice) and carbonated drinks, cocoa, coffee
- fried foods
- meat, fish, mushroom broths
- pork, lamb, goose, duck
- smoked meats, canned food, sausages
- pickles, marinades, spices, mushrooms
- white cabbage, sorrel, spinach, lettuce, radishes, turnips, onions, rutabaga, legumes, raw ungrated vegetables and fruits, cranberries
- pastries, black bread
- confectionery, chocolate, ice cream, jam, creams
- lard, cooking fats
- cold food and drinks
A qualified nutritionist will help you think through the basics of nutrition for chronic pancreatitis, create a diet and take into account the wishes and habits of the patient.
Nutrition and diet
In the first few days, fasting is necessary; you can only drink water - purified without gas, or boiled. In the future, the diet is gradually expanded, table No. 1a is prescribed, as in case of exacerbation of gastric ulcer. Protein-rich foods are allowed - lean meat - beef, rabbit, turkey, in the form of steamed meatballs or soufflé, boiled lean fish, steamed protein omelet, low-fat cottage cheese, pureed viscous porridge. Drinks you can drink include tea, rosehip infusion, and blackcurrant compote.
All dishes are prepared either steamed or boiled, carefully chopped or pureed. Portions are small, not exceeding the amount that fits in one handful. The number of meals is from 6 to 8 times a day.
Extractive substances that enhance secretion - strong broths, mushrooms, coffee, cocoa, chocolate, marinades, smoked meats - are excluded from the menu. All foods that require effort from the pancreas - fatty, fried, salty, spicy, seasonings and spices, canned food, cream, sour cream, fatty cottage cheese, lard - will have to be put aside. You can't eat fast food, soda, colorful candies and chocolate bars, chips, crackers, nuts - everything we're used to snacking on on the go. An unconditional, categorical, non-discussable taboo on alcohol. And for beer. And for non-alcoholic drinks, too.
Typically, diet solves about 70% of the problems that arise during exacerbation of chronic pancreatitis. Once you give the gland rest, the inflammation will begin to subside. The main thing is to take the necessary time, and not “break down” when everything starts to get better and stops hurting.
FAQ
Does the pancreas die in chronic pancreatitis?
Chronic pancreatitis is a disease characterized by inflammation and dystrophy with subsequent development of connective tissue in the organ and disruption of digestive and endocrine function. The “death” of the gland is called pancreatic necrosis and occurs in acute pancreatitis, being a deadly condition
Why does pancreatitis develop if I don’t drink?
Indeed, in most cases, the development of pancreatitis is caused by the effect of alcohol, but there are other factors: cholelithiasis, liver diseases characterized by impaired formation and outflow of bile, diseases of the stomach and duodenum, heredity, a malfunction in the immune system, impaired blood supply to the organ, background diseases: viral hepatitis, hemochromatosis, cystic fibrosis, etc.
Can pancreatitis be cured?
Chronic pancreatitis is called chronic because it cannot be completely cured, but correct medical tactics can achieve long-term remission.
Can pancreatitis lead to the development of diabetes?
Yes, a long course of pancreatitis can lead to the development of not only a violation of the digestive function of the pancreas, but also a change in the endocrine function with the development of diabetes mellitus, especially in the presence of a hereditary predisposition to diabetes mellitus.
Is it important to follow a diet for pancreatitis?
Diet is a fundamental factor in achieving remission.
Pathogenesis of the disease
Inflammatory phenomena in the pancreas gradually lead to degenerative changes in its structure, tissue sclerosis and obliteration of the ductal system. This process usually occurs in waves. The exacerbation is replaced by remission, instead of the glandular tissue that produces enzymes, connective tissue appears. Gradually, enzymes become insufficient; first of all, the exocrine function of the pancreas (production of digestive enzymes) decreases, and then the endocrine function (decreased insulin production).
Symptoms of pancreatic enzymatic insufficiency appear when normal pancreatic tissue is damaged by 90%.
Triad of symptoms of chronic pancreatitis
- pancreatic calcification;
- diabetes;
- steatorrhea is characteristic of an advanced stage of the disease. Steatorrhea occurs when lipase production by the pancreas falls below 16% of its normal level.
Impaired processing and absorption of nutrients in chronic pancreatitis leads to poor absorption of proteins, fats and vitamins. As a result, exhaustion, asthenia, and metabolic disorders of bone tissue and the blood coagulation system may develop.
Treatment stories
Story No. 1
Patient X., 52 years old, came to the EXPERT Clinic with complaints of girdling pain after eating fatty foods and a small amount of alcohol, nausea, and loose stools. From the anamnesis it is known that discomfort in the area above the navel with loose stools was observed for several years due to dietary errors, but after following a strict diet they disappeared without a trace. The woman was not examined for this reason. This is the first time that real complaints have arisen. In addition, 20 years ago, during pregnancy, the patient was told about the presence of thick bile on ultrasound. The patient was not examined further, as nothing bothered her. During a laboratory and instrumental examination, changes in blood tests were revealed: increased ESR, pancreatic amylase activity, and ultrasound revealed multiple stones in the gall bladder. After pain relief, the patient was referred for planned surgical treatment - removal of the gallbladder. After a successful operation, the patient continues to be monitored by a gastroenterologist, follows dietary recommendations, has no complaints, and her indicators have returned to normal.
Story No. 2
Patient B., 56 years old, applied to the EXPERT Clinic with complaints of periodic intense pain syndrome of a shingles nature for no apparent reason, accompanied by nausea and diarrhea. At the previous stage of the examination, diffuse changes in the structure of the pancreas were identified, which was regarded as chronic pancreatitis. The patient led a healthy lifestyle, did not drink alcohol or fatty foods. The prescribed treatment with enzyme preparations did not have a significant effect. When trying to find out the cause of the development of pancreatitis, the gastroenterologist at the EXPERT Clinic ruled out a number of diseases that could lead to the development of chronic pancreatitis (gastrointestinal tract disease, peptic ulcer, iron metabolism disorder, etc.) and drew attention to an immunological shift in laboratory tests. This served as the basis for an in-depth immunological examination, which made it possible to establish that the cause of damage to the pancreas was a malfunction of the immune system - autoimmune pancreatitis. A pathogenetic treatment was prescribed that influenced the mechanism of development of the disease - glucocorticosteroids according to a regimen, against the background of which, during a control examination, the signs of immune inflammation were eliminated. Currently, the patient is receiving long-term maintenance therapy under the supervision of a supervisor and has no complaints. During control ultrasound of the abdominal organs, no signs of pancreatic edema were detected.