Stomach diseases account for 35% of all gastroenterological pathologies. The bulk of these diseases are chronic, with regular exacerbations and remissions. This is primarily chronic gastritis, which accounts for 60-85% of all gastric pathology, and peptic ulcer disease, which affects 10% of the world's population.
According to the Sydney International Classification (1990), there are acute gastritis, chronic and special forms of gastritis (reactive, radiation, lymphocytic, eosinophilic, giant hypertrophic, granulomatous, etc.)
Acute gastritis
Acute gastritis is an acute inflammation of the gastric mucosa, which occurs under the influence of various exogenous and endogenous factors and is accompanied in some cases by dystrophic or even necrotic changes.
Exogenous factors causing acute gastritis are the use of non-steroidal anti-inflammatory drugs (aspirin, indomethacin, etc.), alcohol, mechanical damage (rough food, foreign bodies), chemical and thermal burns (alkalies, acids, hot food), bacterial (food toxic infections ).
Endogenous factors: gastric ischemia, systemic infections (salmonellosis, dysentery, typhoid fever); infectious diseases (flu, pneumonia); shock, severe stress; autointoxication in renal and liver failure; metabolic disorders of various origins.
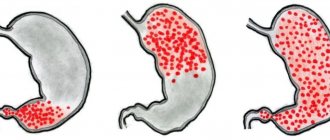
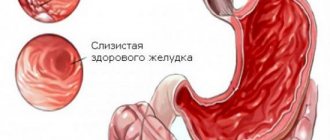
The most common morphological form of acute gastritis is catarrhal gastritis. With catarrhal gastritis, the gastric mucosa is thickened, swollen, hyperemic, its surface is densely covered with mucous masses, there are small multiple hemorrhages and erosions.
Treatment of catarrhal gastritis should begin with gastric lavage with warm water and the administration of adsorbent substances (activated carbon, clay, sorbents, etc.). If necessary, antibacterial drugs are indicated (enteroseptol 0.5 g 3 times a day, clarithromycin 0.5 g 2 times a day for 2-3 days, etc.).
Diet is of great importance. During the first two days, it is recommended to refrain from eating. During the day you need to drink 1.5-2 liters of liquid (warm tea with lemon, rosehip infusion, rice or oatmeal broth, etc.). On the 2-3rd day, mucous soups, cream, milk and dairy products, semolina and pureed rice porridge are recommended. On the 4-5th day - low-fat meat or fish broth, boiled chicken, fish, steamed cutlets, mashed potatoes, crackers. In the future, the diet is expanded.
First of all, it is necessary to eliminate the cause of gastritis. Infusion therapy, antacids, H-2 histamine receptor antagonists, omeprazole (omez), sucralfate are prescribed.
To eliminate pain, anticholinergics are prescribed: platiphylline hydrotartrate, 1 ml of 0.2% solution subcutaneously; gastrocepin 2 ml of 0.5% solution intramuscularly; papaverine hydrochloride 1 ml 2% solution subcutaneously.
The prognosis for acute catarrhal gastritis in the case of timely treatment is favorable. In the vast majority of cases, recovery occurs.
Chronic gastritis
Chronic gastritis is a group of long-term recurrent diseases of the stomach, which are morphologically characterized by inflammatory, dystrophic changes in the gastric mucosa, accompanied by a violation of the physiological regeneration of epithelial cells and, as a result, progressive atrophy of the specialized glandular epithelium and a secondary disorder of the motor and often endocrine function of the stomach. Chronic gastritis is the most common disease. According to biopsy studies confirming the diagnosis of chronic gastritis, it occurs in more than half of those examined in the population. Incidence rates in individual population groups vary widely; the older people are, the more often they are diagnosed with gastritis. Up to 60% of the population has some form of gastritis under the age of 50, and 95% before the age of 70. About 90% of cases of chronic gastritis are associated with Helicobacter pylori, and only about 5% are due to autoimmune atrophic gastritis, 5% to special forms of gastritis. Helicobacter-associated non-atrophic (superficial) gastritis (type B) is the most common variant, accounting for 85-90% of all forms of chronic gastritis. In clinical practice, gastritis (gastroduodenitis) associated with Helicobacter pylori infection predominates, which is detected in 100% of cases. Currently, all leading gastroenterologists in the world recognize the etiological role of H. pylori in the development of non-immune gastritis. In previous classifications, this type of gastritis was designated as superficial gastritis.
Chronic non-atrophic (superficial) gastritis (type B), associated with HP infection. With prolonged persistence of H. pylori infection in the gastric mucosa, active chronic gastritis develops. It is often associated with chronic duodenitis and ulcer-like dyspepsia. In most cases, inflammatory-atrophic changes appear at a young age, localized mainly in the upper part of the stomach against the background of normal or increased secretion of hydrochloric acid. Almost half of the adult population suffers from chronic gastritis, but only 10-15% regularly present complaints associated with this disease. In other people, the disease occurs either without any clinical manifestations or with minimal symptoms, and they do not make an appointment with a gastroenterologist.
Main symptoms
The clinical manifestations of non-atrophic gastritis are practically no different from other forms of the disease:
- pain in the epigastrium, often after eating;
- vomiting at the height of pain, bringing relief;
- heartburn;
- decreased appetite;
- sour taste in the mouth;
- belching sour;
- whitish coating on the tongue;
- constipation, less often - diarrhea.
Superficial inflammation often occurs with subtle symptoms, which makes early detection and treatment of the disease difficult.
Note. Rarely, with antral gastritis without atrophic changes, an atypical pain syndrome occurs, simulating the clinical picture of a duodenal ulcer - “hunger” pain that goes away after eating. But, unlike ulcers, with gastritis there is no night pain and it is not characterized by seasonality of symptoms.
Dietary regime
During an exacerbation of an active inflammatory process, a gentle diet is prescribed. The diet should ensure the maximum reduction in mechanical, chemical and thermal irritation of the gastroduodenal mucosa while maintaining the physiological completeness of the diet.
Products and dishes that have a strong irritating effect on the gastric mucosa are excluded: raw vegetables and fruits containing coarse plant fiber, fried foods, pickles, smoked foods, marinades, hot seasonings, strong coffee, spices, as well as foods that are poorly tolerated by patients.
Most patients with chronic gastritis during a period of stable remission are advised to eat a nutritious diet with the exception of foods that can provoke an exacerbation. Includes lean ham, pureed fruits, large quantities of vegetables, herbs, fruit and vegetable juices, and soft apples.
It is necessary to avoid the consumption of alcoholic beverages, including beer, and to stop smoking, since a correlation has been identified between smoking and the appearance of intestinal-type metaplasia of the gastric mucosa.
Regular, split meals up to 5-6 times a day are very important. It is important to monitor what medications the patient is taking to treat concomitant diseases and, if possible, discontinue those that damage the mucous membrane. If such drugs cannot be discontinued, then you should try to reduce their daily dose. Sometimes, to reduce the risk of drug-induced damage to the gastric mucosa, long-term gastroprotectors are prescribed to protect the gastric epithelium from the effects of drugs and other aggressive factors.
As the exacerbation subsides, it is necessary to expand the diet, taking into account the patient’s taste and habits.
Causes of inflammation
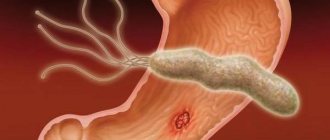
The most common cause of gastritis is Helicobacter pylori. This is a hydrochloric acid-resistant bacterium that attacks the inner lining of the stomach. According to statistics, Helicobacter pylori infection causes inflammation in 90% of cases. As a rule, Helicobacter pylori multiplies in the antrum, since this is where the pH level is most comfortable for it. That is why chronic non-atrophic antral gastritis is most often detected.
More rare causes of the development of non-atrophic inflammation include:
- other infectious agents - viruses, bacteria, fungi;
- nutritional factor, i.e. improper, irregular nutrition;
- reflux of bile from the duodenum into the stomach cavity - biliary reflux;
- prolonged stress;
- smoking;
- alcohol abuse;
- the use of anti-inflammatory, antipyretic drugs, analgesics;
- changes in hormonal levels;
- reduced blood supply to the stomach in diseases of the heart and blood vessels.
The listed factors can cause an inflammatory reaction even with short-term exposure. In some cases, for complete recovery it is enough to simply eliminate the cause of the disease.
Drug therapy
Patients with asymptomatic chronic gastritis in most cases do not require special drug treatment. In these cases, following general recommendations may be sufficient.
For chronic gastritis (type B), associated with H. pylori, drug treatment is reduced to removing Helicobacter from the gastric mucosa with the help of antibacterial drugs, eliminating inflammation, and correcting the secretory function. These effects help prevent the progression of the disease, and in some cases, reverse the development of the process.
Anti-Helicobacter therapy is a system that includes both first-line and reserve (second-line) therapy in case the first-line treatment is ineffective.
H.pylori is sensitive to bismuth drugs, amoxicillin, tetracycline, clarithromycin, metronidazole. To achieve the eradication effect, the simultaneous administration of at least two anti-Helicobacter drugs is necessary. The administration of proton pump inhibitors by increasing the pH of gastric juice creates favorable conditions for the effects of amoxicillin.
As first-line therapy, proton pump blockers are used (omeprazole (omez) 20 mg, lansoprazole 30 mg, rabeprazole 20 mg, esomeprazole 20 mg) 2 times a day in combination with clarithromycin (clacid) 500 mg 2 times a day and amoxicillin 1000 mg 2 times a day for at least 7-14 days.
If there is no eradication of H. pylori after the above treatment, you should move on to the second (backup) four-component treatment regimen (quadruple therapy).
Quad therapy makes it possible to remove H. pylori strains that are resistant to known antibiotics. It includes one proton pump inhibitor, a bismuth salt preparation and two antimicrobial drugs:
- proton pump blockers (omeprazole (omez) 20 mg, lansoprazole 30 mg, rabeprazole 20 mg, esomeprazole 20 mg) 2 times a day;
- bismuth preparations (colloidal bismuth subcitrate or bismuth subsalicylate 120 mg 4 times a day);
- tetracycline 500 mg 4 times a day;
- Metronidazole 500 mg 2 times a day.
In all regimens, metronidazole can be replaced with furazolidone 0.1 g 4 times a day or 0.2 g 2 times a day. The duration of treatment with a four-component regimen is 7-14 days. It is used if there is no effect from first-line therapy after 1-1.5 months.
At the same time, for atrophic gastritis with reduced acid-producing function of the stomach, the following drugs are included as the basic agent of a three-component scheme: - bismuth tripotassium dicitrate (de-nol) 120 mg 4 times a day, which is highly effective against H. pylori and cytoprotective properties that protect the gastric mucosa; — clarithromycin 500 mg 2 times a day; amoxicillin 1000 mg 2 times a day for 7 days.
The most important
Non-atrophic gastritis is the initial stage of chronic inflammation of the stomach. Characterized by mild clinical symptoms. The disease may be asymptomatic. The main cause of the disease is Helicobacter pylori infection. In second place are autoimmune processes. Provoking factors in the occurrence of pathology include bad habits, dietary errors, and long-term antibiotic therapy.
Ignoring clinical symptoms can lead to the transition of an acute process to a chronic one. The disease is highly treatable. Inflammation can be eliminated with the help of medications, nutritional therapy and folk recipes. Treatment of type B gastritis has a positive prognosis. The main thing is to identify the pathology in time and follow the doctor’s recommendations.