The text is presented for informational purposes only. We strongly urge you not to self-medicate. When the first symptoms appear, consult a doctor. We recommend reading: “Why you can’t self-medicate?”
Creatorrhea is the presence of undigested muscle and connective tissue fibers in the stool. The symptom develops when there is insufficient supply of enzymes that break down protein into the duodenum. Creatorrhea is evidence that protein digestion is impaired.
Steatorrhea and amilorrhea are often detected together with creatorrhea.
Medical products (drugs, medicines, vitamins, dietary supplements) are mentioned for informational purposes only. We strongly do not recommend using them without a doctor's prescription. We recommend reading: “Why can’t you take medications without a doctor’s prescription?”
Causes
They lie in various diseases of the digestive canal:
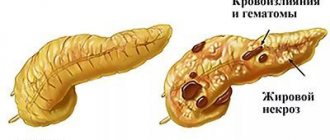
- Chronic inflammation of the pancreas or pancreatitis - the process leads to exocrine insufficiency of the gland, when little digestive juice is produced. The concentration of the main enzymes, primarily trypsin and chymotrypsin, decreases sharply. Some gland cells die, and the organ cannot perform its function sufficiently. The situation can only be corrected by lifelong use of replacement medications.
- Gastritis or inflammation of the gastric mucosa, especially chronic, when the synthesis of hydrochloric acid is disrupted and its secretion is reduced. The available hydrochloric acid is simply not enough to completely break down food protein.
- Putrefactive dyspepsia is a condition when protein foods cannot be digested properly. The intestines are in a constant state of inflammation and are unable to break down the protein that comes with food, so it is excreted undigested.
- Ahilia is a rather rare condition when there is neither hydrochloric acid nor pepsin in the gastric juice; there is simply nothing to break down the protein. Because of this, food rots in the intestines and profuse diarrhea occurs. Achilia is not an independent disease, but accompanies severe infections (tuberculosis, anemia, diseases of the nervous system), and occurs during severe stress and mental illness;
- Acceleration of the movement of the food bolus through the intestines, due to which substances are excreted unchanged. This happens with infections and disturbances of normal microflora.
Associated symptoms
Creatorhea is rarely found in isolation. Much more often, the process of digesting food is completely disrupted, all components are poorly broken down. Creatorhea is usually accompanied by:
- lientorrhea - the appearance of pieces of undigested food in the stool;
- steatorrhea – release of undigested fats, saponification of feces;
- amilorrhea - the release of starch, which indicates a violation of the absorption of carbohydrates;
- Sometimes dysbacteriosis is an additional finding, but this is not necessary.
Diagnostics
During an external examination, the gastroenterologist draws attention to the lack of body weight of the patient with amilorrhea. Dryness and flaking of the skin, brittle nails, and jams are often detected, which indicates vitamin deficiency. The frequency and nature of stools, dietary habits, against which the symptoms appeared, are determined. To determine the causes of amilorrhea, laboratory and instrumental methods are used:
- Stool tests.
The coprogram contains an increased content of starch grains, neutral fats and undigested muscle fibers. To clarify pancreatic functions, the level of fecal elastase is measured. If there is a possible intestinal infection as the cause of amilorrhea, stool culture is indicated. - Functional tests.
To evaluate enzymatic activity, probe and probeless methods are performed. The pathology of the organ, manifested by amylorhea, is evidenced by an insufficient increase in the volume of secretions and the level of bicarbonates after drug stimulation. As a screening method, a blood test for amylase and lipase is performed. - Instrumental visualization.
To study the structure, contours and echogenicity of the organ, an ultrasound scan of the pancreas is performed. For a more detailed study of the parenchyma, a patient with amilorrhea needs an MRI. To exclude malignant neoplasms, selective angiography is informative. The condition of the pancreatic ducts is examined using ERCP. - Fibrogastroduodenoscopy.
The technique is recommended for suspected hyperacid gastritis, which provokes amilorrhea. With EGDS, specific inflammatory changes in the gastric wall, erosions are noticeable, and sometimes ulcerative defects are found. To change the level of hydrochloric acid secretion, intragastric pH-metry is performed. - Biopsy.
An invasive study with sampling of pancreatic tissue is necessary to assess the degree of fibrosis and destruction of the parenchyma, and to identify damage to the insular apparatus in patients suffering from amylorhea. The biopsy technique is very important for understanding the prognosis of the disease and choosing treatment tactics.
Starch grains in coprogram
Diagnosis of causes
A full examination by a gastroenterologist is necessary. Depending on the prevailing clinical symptoms, the following studies are prescribed:
- determination of the level of pancreatic enzymes in the blood and urine - primarily amylase and lipase;
- determination of elastase-1 or amylase isoenzyme in the blood (helps to clarify the severity of inflammation);
- determination of trypsin in blood serum;
- detailed coprogram or stool analysis;
- determination of the content of pancreatic enzymes in the secretion of the duodenum;
- determination of elastase-1 in stool (fecal);
- Ultrasound of the abdominal organs;
- FGDS;
- colonoscopy;
- X-ray of the stomach and intestines with contrast;
- endoscopic retrograde cholangiopancreatography or ERCP - endoscopic examination of the biliary tract, gallbladder and pancreatic ducts;
- CT or MRI cholangiopancreatography – layer-by-layer examination of the gallbladder and pancreas;
- determination of glucose levels and glucose tolerance test.
Treatment
Treatment is always comprehensive, aimed at all aspects of the pathological process.
Diet
For pancreatitis, the best medicine is hunger.
3-5 days of complete fasting are enough for the inflammation to subside. You can drink pure water or weak tea without sugar, a decoction of herbs (if the patient has taken them before, there is no allergy to them and the herbs are well tolerated - chamomile, St. John's wort and the like). You need to start eating food gradually, listening to your feelings. The food should be soft, warm and pureed at first. Protein foods are either excluded completely - for a short period, or their quantity is significantly limited. Food should be taken in small portions every 3 - 4 hours, food should only be fresh. Reheating yesterday's dishes is not allowed.
| Recommended Products | Not Recommended Products |
|
|
Drugs
The basis of treatment is digestive enzymes. Antibiotics are sometimes used to suppress inflammation.
The following groups of enzyme preparations are used:
- medications containing pancreatin - Creon, Penzital and the like;
- preparations containing pancreatin together with bile components, as well as hemicellulase - Festal, Enzistal, Digestal, Normenzim, Biofestal, Panolez;
- herbal preparations containing papain, rice fungus extract and others - Oraza, Solizim, Pepfiz;
- combination preparations with pancreatin and plant enzymes - Wobenzym, Phlogenzyme, Mercenzyme;
- disaccharidases – Lactase.
Antibiotics are selected individually depending on the result of the coprogram and the clinical picture.
Traditional methods
Traditional medicine plays a supporting role, since all homemade herbal preparations have an extremely low concentration of active substances, and it takes time for them to accumulate and take effect.
Folk remedies can complement the main treatment. The following are used:
- tincture of kryphea - a special type of moss, the Amur species is listed in our country in the Red Book as endangered, the tincture is made from kryphea multidirectional (grows in the Balkans, the Caucasus and the Krasnodar region);
- chicory drink;
- oatmeal jelly;
- potato juice;
- barberry decoction;
- flax seed decoction;
- a decoction of equal parts of immortelle, wormwood and chamomile;
- royal jelly.
Publications in the media
Chronic diarrhea (chronic diarrhea) is systematically profuse stool, the weight of which exceeds 300 g/day, lasting more than 3 weeks.
Etiology and pathogenesis
• Exudative diarrhea - bacterial and inflammatory diseases of the colon with damage to the epithelium, the formation of ulcers, crypt abscesses •• Inflammatory diseases of the colon - ulcerative colitis, Crohn's disease, ischemic colitis, radiation colitis, microscopic colitis, diverticulitis •• Infectious diseases - enterotoxins Shigella, Salmonella, Clostridium difficile, Cryptosporidium, Campylobacter, Neisseria gonorrhoeae, Yersinia, Entamoeba histolytica, Lamblia intestinalis, Strongyloides stercoralis •• Malignant neoplasms of the intestine •• Ischemic intestinal diseases.
• Osmotic diarrhea - accumulation in the intestinal lumen of non-absorbable osmotically active soluble carbohydrates that undergo bacterial fermentation with the formation of volatile fatty and lactic acids •• Diseases associated with enzyme defects - primary, secondary fermentopathy: lactase deficiency, celiac disease •• Functional failure of the stomach, pancreas glands, liver and biliary system •• Anatomical damage to the intestine: post-resection and vascular diseases •• Immune diseases •• Drug malabsorption - mannitol, sorbitol, lactulose, pectins, anthraquinones, antimetabolites, cytostatics, bile acids.
• Secretory diarrhea - pathological secretion of fluid into the intestine due to excessive secretion of Cl–, malabsorption of Na+, K+ •• Enterotoxins Vibrio cholerae, Escherichia coli, Bacillus cereus; various viruses (adenoviruses, coronaviruses, etc.) •• Hormones (Vipoma, Werner-Morrison watery diarrhea, Zollinger-Ellison syndrome, serotoninoma, somatostatinoma, etc.) •• Other causes: malabsorption of bile acids, accumulation of excess fatty acids, idiopathic secretory diarrhea (hypersecretion of Cl–), drug-induced diarrhea due to the use of laxatives (bisacodyl, laxacodyl, lactulose, phenolphthalein, castor oil).
• Motor diarrhea - diarrhea due to spastic contractions of the intestines; normalization of stool is typical during fasting, taking drugs that inhibit peristalsis, and abolishing laxatives •• Endocrine pathology - hyperthyroidism, medullary thyroid cancer, thyroid C-cell adenoma, carcinoid syndrome •• Visceral neuropathy - vagotomy, sympathectomy, diabetic neuropathy, amyloid neuropathy , scleroderma •• Diseases of the brain and spinal cord - tumor, syringomyelia, amyotrophic lateral sclerosis, tabes spinal cord •• Anatomical damage associated with diseases or operations on the gastrointestinal tract: dumping syndrome, short bowel syndrome, irritable bowel syndrome, systemic sclerosis • • Drug effects - antacids containing MgSO4, PO42–, cholinomimetic agents.
Clinical picture • Frequent loose stools, abdominal pain, tenesmus, rumbling sensation, transfusion, bloating, flatulence, possible fever, weight loss •• Exudative diarrhea - loose stools, often with blood and pus •• Osmotic diarrhea - copious stools (polyfecality) , may contain a large amount of semi-digested food residues (steatorrhea, creatorrhea, etc.) •• Secretory diarrhea - painless, profuse watery diarrhea (more than 1 l) •• Motor diarrhea - moderate volume of feces (up to 500 ml/day), presence in of undigested residues • See also Malabsorption syndrome.
Laboratory research methods • Analysis of peripheral blood - identifying signs of malabsorption syndrome: total protein, albumin, cholesterol, plasma electrolytes, vitamins B12, D, folic acid, etc. (see Malabsorption syndrome) • Coprological examination •• Culture to isolate pathogenic bacteria and determination of sensitivity to antibiotics. The results are positive in 40% of patients with fever and leukocytes in the stool •• Fecal microscopy for the presence of helminths and their eggs (three times required) •• Occult blood test •• Sudan black staining to detect steatorrhea •• Wright or methylene blue staining for detection of leukocytes, which indicates invasive infectious causes of diarrhea. Staphylococcus aureus, Clostridium perfringens and Entamoeba histolytica can be isolated without the presence of leukocytes in the stool. Irritable bowel syndromes, malabsorption and laxative abuse also do not lead to the appearance of cellular elements of inflammation •• Latex agglutination test to detect Clostridium difficile.
Special research methods • Irrigography • Rectocolonoscopy (proctosigmoidoscopy) • Biopsy to detect pathological changes in the intestinal wall at the histological level.
Differential diagnosis • Differentiation of functional and organic disorders • Determination of the cause of diarrhea.
TREATMENT
Diet • Diet No. 4b. Helps inhibit peristalsis, reduce the secretion of water and electrolytes into the intestinal lumen; the principle of mechanical and chemical sparing. In the acute period, it is necessary to exclude foods that enhance the motor-evacuation and secretory functions of the intestine • Elimination diets for enzymatic deficiency - gluten-free, alactose, etc.
Eubiotics • Baktisubtil - 1 capsule 2-3 times a day 1 hour before meals • Enterol - 1-2 capsules 2-4 times a day, course of treatment - 3-5 days. Particularly effective for diarrhea that develops after antibacterial therapy • Hilak-forte - 40-60 drops 3 times a day; after 2 weeks, the dose of the drug is reduced to 20–30 drops 3 times a day and treatment is continued for another 2 weeks • Bifidobacterium bifidum, Bifidobacterium bifidum + Escherichia coli, Linex, Lactobacillus acidophilus are usually prescribed after antibacterial therapy for 1–2 months.
Symptomatic remedies • Diosmectite - 3 g (1 sachet) 3 times a day 15–20 minutes before meals in the form of a mash (the contents of the sachet are dissolved in 50 ml of water) should be taken separately from other drugs • Herbal medicine - herbal teas (eucalyptus, chamomile, alder fruits, oak bark, cinquefoil, barberry).
Regulators of motility • Loperamide - for acute diarrhea, first 4 mg, then 2 mg after each case of loose stool (no more than 16 mg/day); If normal stool appears and there is no bowel movement within 12 hours, the drug should be discontinued.
Therapy of various types of diarrhea • Secretory diarrhea - secretion inhibitors (octreotide) • Osmotic diarrhea - absorption stimulants (octreotide, riodipine), anabolic hormones, digestive enzymes, complex metabolic therapy • Exudative diarrhea - sulfasalazine, mesalazine, GCs • Motor diarrhea - motility modulators: loperamide, trimebutine; psychotherapy, treatment of the underlying disease.
Rehydration therapy is mainly indicated for acute diarrhea; in chronic cases it is prescribed if necessary.
ICD-10 • A09 Diarrhea and gastroenteritis of presumably infectious origin • K52.9 Non-infectious gastroenteritis and colitis, unspecified
Note. Medicines that cause diarrhea: laxatives; antacids containing magnesium salts; antibiotics (clindamycin, lincomycin, ampicillin, cephalosporins), antiarrhythmic drugs (quinidine, propranolol), digitalis preparations, drugs containing potassium salts, artificial sugar (sorbitol, mannitol), chenodeoxycholic acid, sulfasalazine, anticoagulants.